 Data: Johns Hopkins University
Data: Johns Hopkins University
The World Health Organization declared the COVID-19 outbreak a pandemic March 11.WHO officials said the number of cases outside China had increased tenfold even as it plateaued there.
“Pandemic is not a word to use lightly or carelessly,” said WHO Director-General Dr. Tedros Adhanom Ghebreyesus. “It is a word that, if misused, can cause unreasonable fear, or unjustified acceptance that the fight is over, leading to unnecessary suffering and death.”
COVID-19 is more severe than seasonal flu, there is no immunity to it and there is no vaccine or treatment, according to Tedros. The flu kills “fewer than 1 percent of those infected,” he said, while as of press time a global average of 3 percent of COVID-19 cases have been fatal. "We know there is virus spread before you develop symptoms, and we know there is a large group that actually is asymptomatic or has such mild cases that they continue to spread the virus."
That percentage is projected to drop to as low as 1 percent, however, as more tests reveal the extent of exposure, according to the Fred Hutchinson Cancer Research Center in Seattle. This has given rise to the widely reported conclusion that COVID-19 is 10 times more lethal than the flu (1 percent versus 0.1 percent in the United States.)
After researchers at Fred Hutchinson found that cases of COVID-19 in the Puget Sound region were doubling every six days, Governor Jay Inslee announced mandatory closure of all schools, public, private and charter, in Pierce, King and Snohomish counties from March 17 to April 24. He expanded the closure to every school in the state the next day, limited in-class sessions at colleges and universities, and extended a ban on public gatherings larger than 250 people.
The Legislature unanimously approved $200 million March 13 to fund state health department purchases of tests and equipment, and set aside $25 million for people missing work due to illness or business closures.
President Trump declared a national emergency later the same day, freeing up federal funds for testing, treatment and equipment, and mobilizing the Federal Emergency Management Agency.
During a press briefing at the White House March 16, the administration’s coronavirus response coordinator, Dr. Deborah Birx, said that people without symptoms may be unknowingly spreading the coronavirus. “We know there is virus spread before you develop symptoms, and we know there is a large group that actually is asymptomatic or has such mild cases that they continue to spread the virus… That’s why we’re asking every American to take personal responsibility to prevent that spread.” “This is a controllable pandemic.”
The word “pandemic” comes from the Greek “pandemos,” meaning “all people.” COVID-19 is now present on every continent except Antarctica. China, South Korea, Iran and Italy account for more than 90 percent of all reported cases, according to the WHO.
“This is a controllable pandemic,” Tedros said. “The idea that countries should shift from containment to mitigation is wrong and dangerous.
“You can’t fight a virus if you don’t know where it is. That means robust surveillance to find, isolate, test and treat every case, to break the chains of transmission,” he said.
“Many people in the U.S. will at some point, either this year or next, get exposed to this virus,” said Nancy Messonnier of the U.S. Centers for Disease Control and Prevention in a briefing March 9.
Most people with COVID-19 will experience only mild symptoms, according to the Tacoma-Pierce County Health Department, though some may require medical attention or hospitalization, particularly the elderly and those with compromised immune systems or underlying health conditions such as heart disease or diabetes.
WHAT IS COVID-19? In December 2019, a previously unknown coronavirus was found to be the cause of an outbreak of viral pneumonia in the city of Wuhan, China.
On Feb. 11, the International Committee on Taxonomy of Viruses named the new virus “severe acute respiratory syndrome coronavirus 2” (SARS-CoV-2) because it is genetically related to the coronavirus responsible for the SARS outbreak of 2003.
SARS, which can cause a severe respiratory illness, was first reported in Asia in February 2003 and quickly spread to two dozen countries before being contained after four months. The outbreak had about a 10 percent mortality rate, but since it was contained did not become a pandemic. There have been no known SARS cases since 2004.
Viruses are named to reflect their genetic structure to facilitate development of tests, vaccines and treatment. The diseases they cause often have different names. Rubeola is the virus that causes measles; HIV causes AIDS; coronaviruses can cause anything from a common cold to pneumonia.
New diseases are named by the WHO because it is responsible for a public response. The WHO announced “Corona Virus Disease 2019” (COVID-19) as the name of the new disease Feb. 11.
President Trump and other politicians have referred to COVID-19 as “the China virus” or “a foreign virus,” repeating some cable TV coverage and social media memes. Tedros said the WHO avoids using geographical disease names to prevent stigmatization and the impact it has on reporting new outbreaks. “Having a (science-based) name matters to prevent the use of other names that can be inaccurate or stigmatizing.”
According to the National Foundation for Infectious Diseases, coronaviruses are a large group of viruses that cause diseases in animals and humans. Human coronaviruses were first identified in the mid-1960s and are closely monitored. They are named for the crown-like spikes on their surfaces.
SARS-CoV-2 appeared in a seafood and poultry market in Wuhan in December 2019. The disease it causes is thought to have come from close contact with an infected animal that has not yet been identified. Research suggests that SARS, MERS and COVID-19 all originated in bats. SARS then spread from infected civets to people, while MERS spread through infected camels to people.
There is no cure for COVID-19 and no vaccine, though according to the National Institutes of Health a vaccine could be ready for so-called Phase I safety testing soon and public distribution within 18 months.
SYMPTOMS There are many similarities in symptoms between COVID-19, the flu and the common cold that makes it difficult to distinguish among them, according to Lisa Lockerd Maragakis, M.D., M.P.H., of John Hopkins Medicine. Symptoms can vary by person, but the main symptoms are fever, cough and shortness of breath, body aches, fatigue and sometimes vomiting and diarrhea, and are believed to appear anywhere from two to 14 days after infection.
Patients who have a fever, cough and shortness of breath should call their health care provider before going to a healthcare facility, according to the Tacoma-Pierce County Health Department.
Itchy, watery eyes are a symptom of allergies, not of flu or COVID-19, according to the Mayo Clinic. Allergies also don’t cause body aches and rarely cause a fever — a main symptom for both the flu and COVID-19.
TESTING The Washington State Department of Health said a big part of slowing the spread of COVID-19 is testing people.
The CDC began screening overseas travelers for coronavirus in mid-January, but their test kits were flawed. One Seattle lab defied federal rules to develop its own test and successfully identified the first COVID-19 patient in the state and country. Wide-scale testing began in the U.S. in mid-March.
DOH received additional testing equipment March 6 and continues to ramp up its facility with a goal of processing 400 samples a day, meaning about 200 people. The University of Washington Virology Lab can process as many as 1,500 tests per day; they said their goal is 5,000 (UW began testing March 4.) Commercial labs across the state are also working to get running and begin processing tests.
Some patients have reported receiving large medical bills for COVID-19 testing and care. Washington state committed to making tests free to uninsured populations, and free of deductibles and co-payments for insured populations.
DOH also said not everyone needs to be tested since there is no medication to treat COVID-19. Anyone with a fever and cough should assume their illness could be COVID-19, report their symptoms, and protect others in the community and household from the disease.
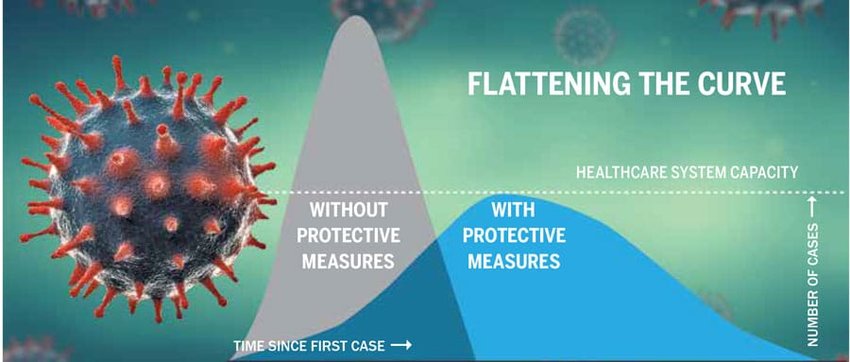
STOPPING THE SPREAD The goal in fighting a large-scale outbreak is to halt the spread, but just slowing it — mitigation — is critical, according to Seattle King County Health Officer Dr. Jeffrey Duchin. Social distancing, quarantining those who may have been exposed, and isolation for those who are infected, all reduce the number of active cases, in turn allowing hospitals time to prepare for more.
The risk of becoming ill from COVID-19 is lower for a young and healthy adult, but the risk of passing it along to someone else and continuing a transmission chain that eventually results in a COVID-19 death in a vulnerable person is much higher, according to TPCHD.
RESPONSE Washington state was among the worst affected by the spread of COVID-19.
Secretary of Health and Human Services Alex Azar told reporters March 10 that the Trump Administration was working directly with Gov. Inslee to ensure the state’s needs are met by tapping into the strategic national stockpile of equipment and medicines reserved for emergencies. Supplies reportedly included surgical masks and gloves, portable respirators and hospital ventilators
“They got half of the shipment from the strategic national stockpile initially, and then when the Vice President (Pence) actually went out to the state of Washington, that’s when the second half of the shipment arrived,” Azar said.
For more information, go to www.tpchd.org or call the Washington State Novel Coronavirus Call Center at 800-525-0127 and press #.
UNDERWRITTEN BY THE FUND FOR NONPROFIT NEWS (NEWSMATCH) AT THE MIAMI FOUNDATION, THE ANGEL GUILD, ADVERTISERS, DONORS AND PEOPLE WHO SUPPORT INDEPENDENT, NONPROFIT LOCAL NEWS